| dc.contributor | Vall d'Hebron Barcelona Hospital Campus |
| dc.contributor.author | Lin, Nancy U. |
| dc.contributor.author | Borges, Virginia |
| dc.contributor.author | Murthy, Rashmi K. |
| dc.contributor.author | Paplomata, Elisavet |
| dc.contributor.author | Hamilton, Erika |
| dc.contributor.author | Antunes de Melo Oliveira, Ana Mafalda |
| dc.contributor.author | Anders, Carey |
| dc.date.accessioned | 2021-08-23T09:56:40Z |
| dc.date.available | 2021-08-23T09:56:40Z |
| dc.date.issued | 2020-08-10 |
| dc.identifier.citation | Lin NU, Borges V, Anders C, Murthy RK, Paplomata E, Hamilton E, et al. Intracranial Efficacy and Survival With Tucatinib Plus Trastuzumab and Capecitabine for Previously Treated HER2-Positive Breast Cancer With Brain Metastases in the HER2CLIMB Trial. J Clin Oncol. 2020 Aug 10;38(23):2610–2619. |
| dc.identifier.issn | 1527-7755 |
| dc.identifier.uri | https://hdl.handle.net/11351/6230 |
| dc.description | Càncer de mama; Supervivència; Tucatinib |
| dc.language.iso | eng |
| dc.publisher | American Society of Clinical Oncology |
| dc.relation.ispartofseries | Journal of Clinical Oncology;38(23) |
| dc.rights | Attribution-NonCommercial-NoDerivatives 4.0 International |
| dc.rights.uri | http://creativecommons.org/licenses/by-nc-nd/4.0/ |
| dc.source | Scientia |
| dc.subject | Mama - Càncer |
| dc.subject | Medicaments antineoplàstics - Ús terapèutic - Eficàcia |
| dc.subject.mesh | Breast Neoplasms |
| dc.subject.mesh | Antineoplastic Combined Chemotherapy Protocols |
| dc.subject.mesh | /therapeutic use |
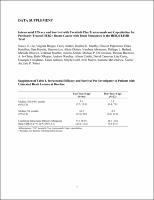
| dc.title | Intracranial Efficacy and Survival With Tucatinib Plus Trastuzumab and Capecitabine for Previously Treated HER2-Positive Breast Cancer With Brain Metastases in the HER2CLIMB Trial |
| dc.type | info:eu-repo/semantics/article |
| dc.identifier.doi | 10.1200/JCO.20.00775 |
| dc.subject.decs | neoplasias de la mama |
| dc.subject.decs | protocolos de quimioterapia antineoplásica combinada |
| dc.subject.decs | /uso terapéutico |
| dc.relation.publishversion | https://ascopubs.org/doi/10.1200/JCO.20.00775 |
| dc.type.version | info:eu-repo/semantics/publishedVersion |
| dc.audience | Professionals |
| dc.contributor.organismes | Institut Català de la Salut |
| dc.contributor.authoraffiliation | [Lin NU] Dana-Farber Cancer Institute, Boston, MA, USA. [Borges V] University of Colorado Cancer Center, Aurora, CO, USA. [Anders C] Duke Cancer Institute, Durham, NC, USA. [Murthy RK] MD Anderson Cancer Center, Houston, TX, USA. [Paplomata E] Carbone Cancer Center/University of Wisconsin, Madison, WI, USA. [Hamilton E] Sarah Cannon Research Institute/Tennessee Oncology–Nashville, Nashville, TN, USA. [Oliveira M] Vall d’Hebron Hospital Universitari, Barcelona, Spain |
| dc.identifier.pmid | 32468955 |
| dc.identifier.wos | 000559991300004 |
| dc.rights.accessrights | info:eu-repo/semantics/openAccess |